
 Back to Labs & Centers
Back to Labs & Centers
Orthopedic Rehabilitation & Biomechanics Laboratory
Rehabilitating traumatic knee injury and preventing knee osteoarthritis
About
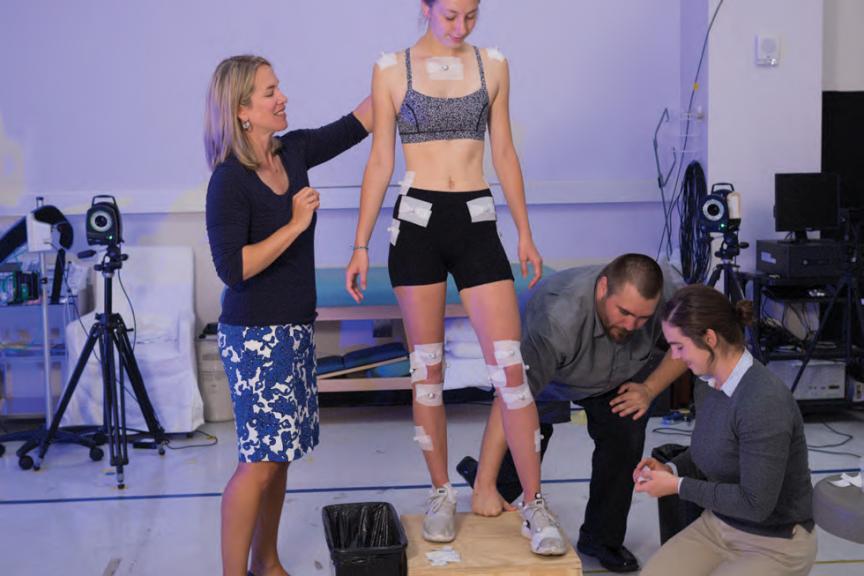
The Orthopedic Rehabilitation and Biomechanics (ORB) Laboratory conducts research focused on the functional limitations and neuromechanical adaptations that occur as a result of joint injury and disease. Traumatic joint injury increases the risk for early onset post-traumatic osteoarthritis. Our work aims to minimize this by identifying novel rehabilitation approaches targeting muscle weakness, biomechanical asymmetries, and functional limitations that result from joint injury. Benefits include reduced risk for re-injury and osteoarthritis, prolonged quality of life, and improved functional ability.
Contact Info
Address
24 Frank Lloyd Wright Drive
Ann Arbor, MI 48106
United States
Phone
Social
Director(s)
Member(s)
Staff
PhD Student(s)
Postdoctoral Fellow(s)
Staff
- Jungsun Moon, MS
- Kylie Saloma, BS
Collaborator(s)
- James Ashton-Miller, PhD, Research Professor, U-M Biomedical and Mechanical Engineering; Senior Research Scientist, U-M Institute of Gerontology
- J. Ty Hopkins, PhD, ATC, Assistant Professor, Brigham Young University Department of Exercise Sciences
- Christopher D. Ingersoll, PhD, ATC, Joe Gieck Professor of Sports Medicine; Professor, University of Virginia Department of Human Services
- Edward M. Wojtys, MD, Medical Director, U-M MedSport Sports Medicine Program; Professor, U-M Department of Orthopaedic Surgery
- Ronald Zernicke, PhD, DSci, Professor, U-M School of Kinesiology